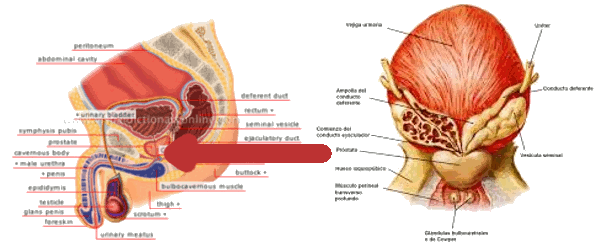
Prostatic Adenocarcinoma
Prostate cancer: the words alone evoke fear. Let us discover what it is together, how it forms, and how we can combat it.
Cancer is a disease characterised by the uncontrolled growth of abnormal cells in the organs. The human body is made up of billions of cells. The cells reproduce by dividing, and in this way growth, or repairing wounds is possible. Sometimes cells reproduce excessively and create a mass called a tumour. Some tumours are benign (non cancerous) and others are malignant (cancerous).
The growth of benign tumours is limited and rarely endangers life, even if it can interfere with the normal bodily functions. Malignant tumours, on the other hand, invade and destroy normal tissues. Metastasis refers to delayed cancerous formations apart from the original cancer. Metastasis occurs when tumour cells separate from the original tumour and spread with the blood or lymphatic circulation to other parts of the body where they establish themselves and reproduce, giving rise to new tumours.
In some cases malignant tumours grow and spread rapidly, and in other cases slowly. For this reason sometimes the development of a large, but not aggressive tumour (defined as “well differentiated”) is more favourable, compared with a small one with uncontrolled growth (“undifferentiated tumours”). One of the places in which tumours develop most frequently in man is the prostate. The widespread opinion that a malignant tumour or cancer is synonymous with certain and imminent death, is absolutely false. In particular, prostate cancer can be easily diagnosed in an early stage, and thus it can be cured; furthermore, because of its feature of very slow growth it permits long survival, even in the large majority of cases in which it was discovered at a stage in which a complete cure was no longer possible.
How Frequent is Prostate Cancer?
The presence of cancer cells in the prostate is rare before 40 years of age (1 %), but with advancing years it becomes extremely common until it reaches close to 100% for men aged over 70. Fortunately, however, only in part of these cases do these cells develop, giving rise to a clinically manifest tumour.
In Italy, prostate cancer represents the 3rd cause of death amongst tumours, with a percentage that is 60% higher in the North of the country. Currently, every Italian aged 65 or more has a 3 % theoretical probability of dying from this condition. In the USA for example, there were 31,900 fatalities in 2000 caused by this disease. The number of tumours discovered using modern methods of prevention has, however, raised a dilemma that is still current: since not all tumours discovered will give problems for the patient, when is it appropriate to act after diagnosis? Diagnosis itself: when is it desirable and useful?
Periodic check-ups help a physician to diagnose prostate cancer early: that is, when it is not only treatable, but curable. The symptoms of prostate cancer are absent or rare in initial stages, and are often associated with those of a co-existing benign prostatic hyperplasia (B.P.H.). Both conditions are common in men, and often cause difficulties with urination with a weak and frequent urination. B.P.H. is the enlargement of that internal part of the prostate close to the urethra. As we have stated in previous sections, it is not cancer. The only accurate way to distinguish between B.P.H. and cancer is a trans-rectal prostate ultrasound scan, combined with the amount of P.S.A., with a biopsy and an examination by a specialist physician. It is reasonable to undergo examinations after the age of 50, or after the age of 40 if relatives have had prostate cancer.
An important video will soon be made available in which we perform a biopsy on 3 patients suspected of having prostate cancer. After sedation for the biopsy, they await the judgement of the histologist in attendance at the time, so they can undergo a cryosurgical procedure if necessary (Link to the Video).
What Causes Prostate Cancer?
The exact cause of prostate cancer is unknown. It is not yet known why, in certain cases, the few cancer cells present in the majority of senior citizens start to proliferate, and give rise to tumours. In its early stages ,the tumour may give no trouble, and then, with the passage of time, as it grows, the tumour starts to compress adjoining parts, such as the urethra for example. This phenomenon obstructs the free flow of urine from the bladder. At this stage of the condition, men urinate more frequently than normal (this is often the first symptom of the disease); sometimes urination is very difficult and even painful.
Other symptoms are the presence of red or white blood corpuscles in the urine or in the sperm. it is important to recall that prostate cancer, especially in the initial stages, can fail to have symptoms of any kind, so that after 40/50 years of age, regular specialist check-ups are recommended. When prostate cancer spreads to adjoining lymph nodes, to the bones or other organs, many men feel bone or joint pain.
What makes Prostate Cancer Grow?
The growth and the normal functioning of the prostate depend on a male hormone: testosterone. Almost all testosterone is produced by the testicles, and a small part is made by the adrenal glands. Testosterone has the same effect on prostate cancer that gasoline has on fire. For as long as the organism produces testosterone, the tumour will grow and spread.
Diagnosis
Physicians use several methods to diagnose prostate cancer.
Rectal exploration in the most common and most ancient system. In this examination, the physician inserts a gloved and lubricated finger into the rectum, feels the rear surface of the prostate through the intestinal wall, and in this way assess its shape and consistency. This procedure is fast and causes minimum disturbance to the patient. Unfortunately, when the physician feels “something” and it turns out to be a tumour, one time out of two the disease is already advanced and can no longer be cured. This is because not all tumours have a shape and consistency that is such that it makes them feel different and thus recognisable, apart from healthy tissue. Furthermore, they are also very often located in the part of the prostate that cannot be touched by the physician’s finger.
Prostate-specific antigen (P.S.A.) is a protein produced exclusively by healthy and diseased prostate gland tissue. This substance increases in the blood when a larger number of gland cells develop in the prostate; diseased, inflamed, or tumorous gland cells produce much more PSA than normal cells. Recent studies have enabled it to be demonstrated that there is a relationship between the volume of BPH and the level of PSA. By means of trans-rectal ultrasound scanning, the individual reference value for each patent can be derived (PSAP: PSA prediction). When the dose of PSA in the blood exceeds the PSAP, a great deal of care is necessary because the presence of carcinomatous cells is highly probable. The reference levels at several analysis laboratories are very high, and thus they can give rise to false optimism; sometimes even with much lower values than those that are deemed normal, significant prostatic adenocarcinomas can be present.
Trans-rectal ultrasound scanning is an examination that enables the value of the PSAP, suspect areas, bladder functioning, the presence of prostatic stones, and the structure of the prostate to be identified, even in the part far from the rectum where the physician’s finger cannot reach through rectal exploration.
During this examination a thin instrument, able to generate ultrasound waves, is inserted in the rectum. Those waves are reflected by the tissues according to their consistency and generate various echoes. The same ultrasound source is able to receive echoes on the way back, and those echoes are then converted into an image that the physician can see on a TV screen.
IN EACH CASE, when the presence of prostate cancer is suspected, there is only one way to be certain of the diagnosis: a biopsy. The physician may take small samples of the prostate using a thin needle. Those samples are examined under the microscope in order to check if carcinomatous cells exist. The safest and most painless method to take prostate samples in suspected areas is via an ultrasound scan, guided trans-rectally. The physician “sees” an ultrasound scan of the areas at risk, and takes samples (targeted ultrasound scan technique). Furthermore, it is possible to take samples of tissue from around the prostate to find out how far the disease has reached (biopsies in stages).
Who Treats Prostate Cancer?
When prostate disorders are suspected the doctor in charge can call upon a specialist, the urologist. The latter is a physician and surgeon trained to diagnose and treat diseases of the urinary and genital apparatus. The urologist will understand if the symptoms of a patient have been caused by B.P.H. or cancer. In certain cases the patient can also be sent to an oncologist (a specialist in the medical treatment of cancer).
How to Choose the Best Treatment?
This text dies not intend to and cannot give complete answers for each and every single problem. Aspects that are too technical have been excluded on purpose. For example there is no reference to staging laparoscopic lymphadenectomy, of destructive prostate resection etc. Experience leads one to state that each treatment option should be discussed and clarified as much as possible between doctor and patient, without necessarily wishing to exclude the closest relatives. Only in this way can everyone make their contribution to the prescribed treatment in such a way as to derive the greatest benefit.
What will Happen to Me?
It is normal to find out about being affected by prostate cancer with anxiety, concern or distress. The same feelings will impact friends and family.
Talking with someone who has already faced these issues can be a way to receive help and encouragement. Experience teaches that with the passage of time, patients discover that even when a complete cure is not possible, prostate cancer is a factor with which it is possible to be at peace, living a normal life. If you so wish, you can ask your doctor to put you in touch with other patients. The patients who belong to our group are encouraged to compare their own experience with other patients, so as to be able to make appropriate therapeutic decisions in the most informed and conscious manner possible.
What are the Classifications for the Stages of Prostate Cancer?
The best care for each individual case can only be set up if the physician manages to determine the stage of the illness. Treatment can vary according to the general condition of the patient, his age and the stage the disease has reached. It is important for the patient to discuss the various possible options with the doctor, and their advantages and disadvantages.
Currently, in Italy, the TNM system is used. That is an international classification system for tumour development according to 3 parameters. Together with Gleason Grading and the PSA test, it is possible to best classify the seriousness of the disease.
T combined with a number from 0 to 4 indicates the tumour volume. N on the other hand concerns the lymph nodes: this is also combined with a number from 0 to 3, where N0 indicates that the regional lymph nodes (that is those that are adjacent and connected to the volume affected by the tumour) have not been impacted by the tumorous cells and are therefore healthy. Codes from N1 to N3 instead indicate the more or less extensive involvement of the lymph nodes; M0 instead indicates the absence of metastasis, with M1 showing their presence instead.
The Gleason scale on the other hand catalogues the aggressiveness and speed of growth of a tumour, with scores from 2 to 10, where the lower numbers correspond to a tumour that Is highly differentiated from healthy cells. After a biopsy, a pathologist will assign a score from 1 to 5 for the cancer formations that are most represented in the sample, and immediately after that a score from 1 to 5 for the less common ones. Their total will form the value on the scale.
Therapy
The statistics and data relating to this item are now out-dated. We are working to update them with the most recent statistics. As regards cryosurgery please see the dedicated page for some information of a general and historical nature:
Radical prostatectomy;
Partial prostatectomy;
Radiotherapy;
Hormone therapy; and
Brachytherapy.